What is red light therapy? In general, light therapy is the effect of light energy of a certain wavelength on tissues to produce a therapeutic effect. The other name for it is photobiomodulation, which we explain below.
Photobiomodulation and other light sources
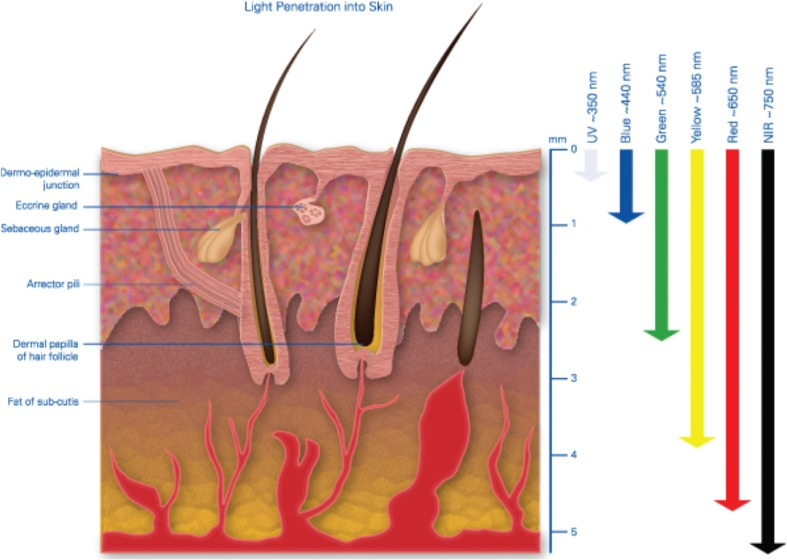
Red light therapy (photobiomodulation) consists of red and near-infrared light waves. Light in red and near-infrared waves penetrates deeper into the skin than other light sources in the spectrum [1].
Photobiomodulation and the sun
If you compare photobiomodulation and the sun, the healing properties of Laser Light are due to these differences:


The sun has positive effects on the body: it produces vitamin D, gives energy, fights depression, kills bacteria, and strengthens the immune system. But because of ultraviolet rays, the sun can also cause sunburn, skin cancer, premature aging, eye damage, etc. Photobiomodulation, on the other hand, has only red and infrared light, which are not harmful to the body.
Photobiomodulation and laser
One name for photobiomodulation is low-level laser therapy (LLLT). But if you compare LLLT to surgical lasers, which can cut, ablate, and coagulate biological tissue with a photothermal effect, LLLT generally does not raise the temperature of macroscopic tissue because of the power density used is well below the threshold required for the photothermal effect.
Effects on the body
Photobiomodulation is a painless and non-invasive procedure. There will be no sound, no vibration, and no heat.
The light in red light therapy, due to its penetrating ability, penetrates deep into the cells (skin, bones, brain, blood). One of the main mechanisms of the action occurs in the mitochondria (the unit of cellular energy within each cell).
Red and infrared LEDs, non-invasively enter the treated tissues in the form of non-ionizing light energy. This energy is absorbed by the mitochondria and converted directly into an energy-carrying molecule used to support cellular metabolism. That is, photobiomodulation stimulates cellular energy production and also reduces oxidative stress (reduces inflammation).
Effectiveness depends on the application of the correct wavelength and density of light entering the target tissues over an appropriate time. Superficial tissues are usually treated using wavelengths between 600 and 700 nanometers (nm). For deeper penetration, wavelengths between 780 and 950 nm are used [2].
Names
Therapeutic photobiomodulation (PBM) has, over the years, received many alternative terms used in one form or another: low-level light therapy (LLLT), red light therapy (RLT), low-level laser therapy, low-intensity laser, low-sensitivity laser therapy, cold laser, non-thermal laser, soft laser, biostimulation laser, photobiomodulation laser or even LED light therapy (LED) and organic LED therapy [3].
In 2015, “photobiomodulation” became the official MeSH term. It was decided that “photobiomodulation” or “photobiomodulation therapy” should be adopted as the preferred term for the future. Besides, the U.S. National Library of Medicine has officially adopted the acronym “LLLT” (Low-Level Laser Therapy), which is the official Medical Subject Heading (MeSH) [6].
History
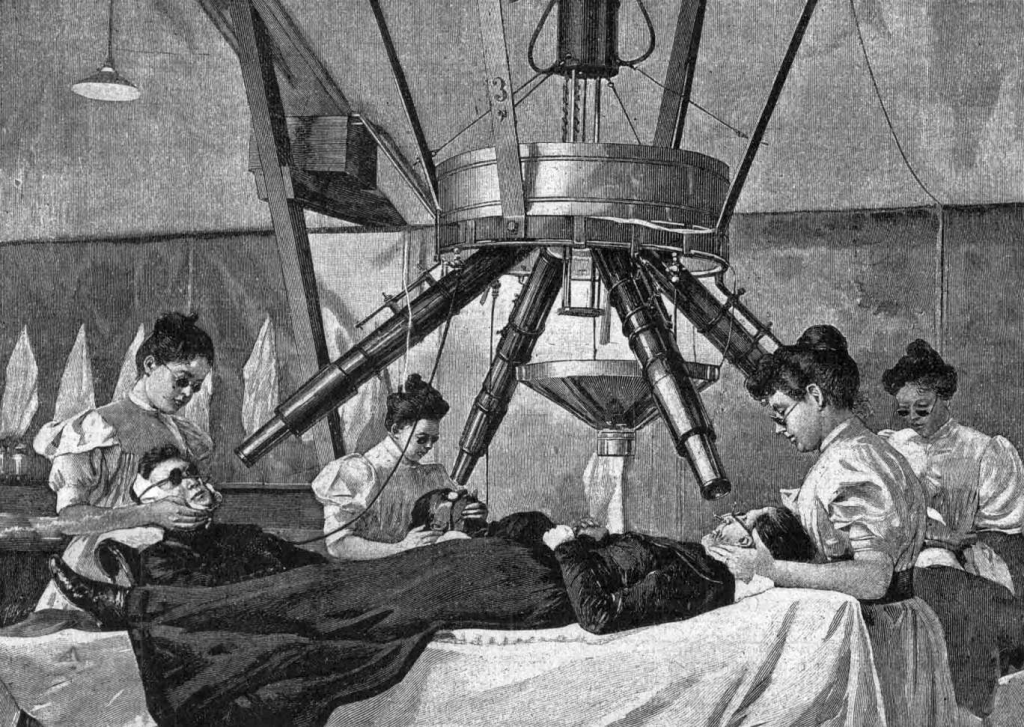
The history of light therapy began back in the late 19th century by Nielson Ryberg Finsen. He first developed a lamp using red and blue light to treat various human diseases, especially lupus vulgaris, for which he received the Nobel Prize in Medicine and Physiology [4].
His pioneering evidence that light could be bactericidal and also stimulate surrounding tissues attracted much attention from doctors and scientists. But because of the lack of a mechanistic explanation, over time, it has been forgotten.
The next important push in the development of light therapy was accidentally made by Dr. Endre Mester in 1967. Mester decided to find out if a laser could cause cancer [5].
The scientist conducted an experiment on mice with shaved hair on their backs. Half of the mice were irradiated with a low-power ruby laser, while the other half was the control.
As a result, the mice did not develop cancer and, to Endre’s surprise, the mice in the irradiated group grew hair faster compared to the control group.
Dr. Endre Mester soon published his results and continued his research. By the 1970s, he was already using low-level laser light to treat people, and he founded the Center for Laser Research in 1974 [7].
The field has since matured, and much has been studied about the mechanistic basis of this therapy, including the key fact that such exposure of tissues and organisms to light can elicit both stimulatory and inhibitory reactions, depending on the light parameters used.
Sources
- Ash, C., Dubec, M., Donne, K. et al. Effect of wavelength and beam width on penetration in light-tissue interaction using computational methods. Lasers Med Sci 32, 1909–1918 (2017).
- Optimising the design of a broad-band light source for the treatment of skin. Clement M, Daniel G, Trelles M. J Cosmet Laser Ther. 2005 Dec; 7(3-4):177-89.
- Michael R. Hamblin, James D. Carroll, Lucas Freitas de Freitas, Ying-Ying Huang M.D., Cleber Ferraresi. Low-Level Light Therapy: Photobiomodulation, 2018.
- Grzybowski A, Pietrzak K. From patient to discoverer–Niels Ryberg Finsen (1860–1904) –the founder of phototherapy in dermatology. Clin Dermatol. 2012 Jul-Aug;30(4):451-5. doi: 10.1016/j.clindermatol.2011.11.019. PMID: 22855977.
- Perera, Judith (19 March 1987). “The ‘healing laser’ comes into the limelight”. New Scientist.
- Anders JJ, Lanzafame RJ, Arany PR. Low-level light/laser therapy versus photobiomodulation therapy. Photomed Laser Surg. 2015 Apr;33(4):183-4. doi: 10.1089/pho.2015.9848. PMID: 25844681; PMCID: PMC4390214.
- Cotler HB, Chow RT, Hamblin MR, Carroll J. The Use of Low-Level Laser Therapy (LLLT) For Musculoskeletal Pain. MOJ Orthop Rheumatol. 2015;2(5):00068. doi: 10.15406/mojor.2015.02.00068. Epub 2015 Jun 9. PMID: 26858986; PMCID: PMC4743666.