The UVB spectrum has properties that are beneficial and harmful to human health. Here we take a closer look at the use of UVB in medicine, answering the following questions:
- What cases are treated with UVB?
- How does the treatment take place?
- What are the risks and methods of reducing them?
- Can UVB therapy be done at home?
What is UV light
Ultraviolet radiation (UV) is electromagnetic radiation invisible to the human eye and occupies the spectral region between visible and X-rays.
The lower limit of the wavelength perceived by human vision is conventionally taken as 400 nm. Ultraviolet light exists between 200 and 400 nm. Therefore, ultraviolet rays are invisible to humans.
To understand the effects of ultraviolet light two parameters are important — wavelength (in nm) and intensity of the radiation (in W/m2 or μW/cm2).
Depending on the wavelength, the ultraviolet spectrum is divided into three regions:
- Long-range — short-wavelength ultraviolet (120-280 nm) or UVC;
- Middle range — mid-wave ultraviolet (280-315 nm) or UVC;
- Near range— long-wave ultraviolet (315-400 nm) or UVA.
Of the ultraviolet radiation reaching, more than 95% is long-wavelength UVA, with a for various reasons small fraction of UVB, and little to no UVC.
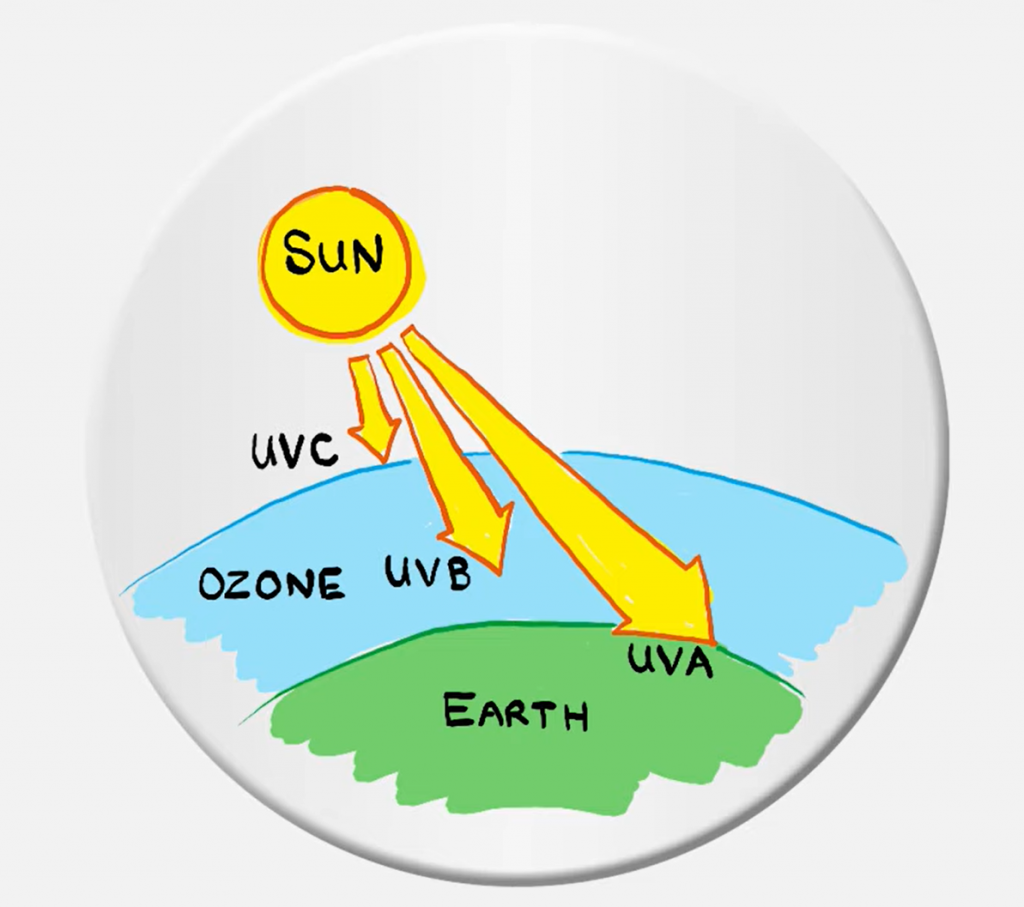
The chemical and biological effects of UV are greater than simple heating effects, and many practical applications of UV radiation derive from its interaction with organic molecules.
Since UVA, UVB and UVC have different radiation intensities, this means that they have different rates of degradation of what they hit.
Using UVB in treatment
The ability to penetrate the skin is proportional to the wavelength of the radiation. Thus, UVA with a longer wavelength can penetrate deep into the skin’s dermis, while UVB is absorbed superficially in the epidermis. In contrast, the energy is inversely proportional to wavelength. UVB has much more energy than UVA, even though UVB reaches the earth’s surface relatively little.
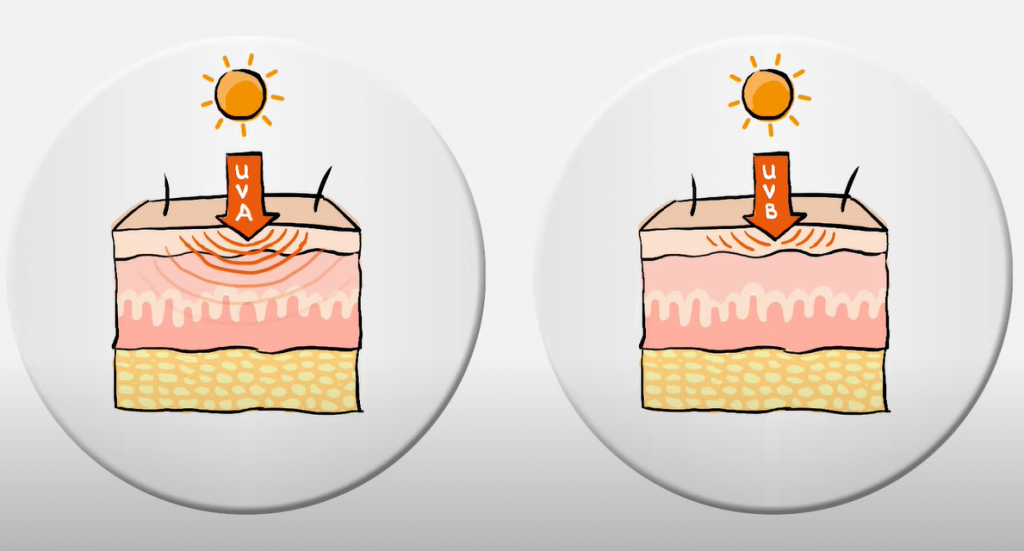
Treatment of many skin conditions
As was pointed out, UVB has a high energy level. So if you have a sunburn, it is mainly because of UVB, not UVA. Nevertheless, it has been successfully used to treat many skin diseases. This is because UVB is inextricably linked to the skin’s immune system. The most popular use of UV-B phototherapy to improve control of psoriasis and eczema symptoms [1, 2, 3].
For moderate to severe psoriasis, proper skincare and application of medication to the affected areas of the skin is not always enough. UV light reduces inflammation and slows down skin cell production. It is estimated that symptoms improve markedly or disappear completely for a time in 50-90 people out of 100 [1].
UVB phototherapy approaches can effectively reduce inflammatory skin conditions. Types of phototherapy in the treatment of skin diseases include broadband UVB (280-320 nm) and narrowband UVB (311-313 nm). This limitation of the light spectrum reduces the risk of side effects.
By weighing the type of disease being treated, the depth of pathology, and the risk of skin carcinogenesis, the physician chooses the amount and type of UV radiation to minimize risks and maximize the immunosuppressive effect of the treatment. Repeated or prolonged light therapy may increase the risk of developing skin cancer.
UVB treatment is quite demanding because it is usually given several times a week in a dermatology clinic or hospital. It can be used alone or in combination with topical (external) medication or pills, or combination with bathing in a solution of table salt or the Dead Sea salt. This proves to be more effective [1]. Home UVB phototherapy is as effective as outpatient UVB phototherapy for mild to severe psoriasis (DOT: Moderate) [4]. Jump to item home UVB phototherapy treatment here.
Vitamin D synthesis
UVB photobiomodulation is used when vitamin D may not be produced, such as when the latitude and time of year negatively affect the amount and quality of solar radiation reaching the Earth’s surface, especially during the winter months [5, 6, 7].
UVB photobiomodulation is also used for various diseases when vitamin D cannot be absorbed effectively. For example, for patients with cystic fibrosis (CF), fat malabsorption syndrome [5], Crohn’s disease [8].
Vitamin D synthesis occurs mostly through exposure to sunlight and a small portion comes from food [6]. Appropriate exposure to sunlight is recommended to get the right amount of vitamin D for the body. However, many people are still deficient in vitamin D for various reasons, which is a serious problem.
To solve this problem, a series of studies were carried out to study artificial lighting, providing rays of ultraviolet light with characteristics similar to those of sunlight [9].
Based on photobiological safety (IEC 62471) lighting was developed UVB LED, providing a safe dosage of UVB. And it was confirmed that vitamin D synthesis in humans can be supported by this type of stimulating diffuse lighting with UVB radiation [9, 10].
Studies published in Scientific Reports show that light from a 293-nm ultraviolet (UV) LED is more effective than sunlight in producing vitamin D3 in skin samples [11].
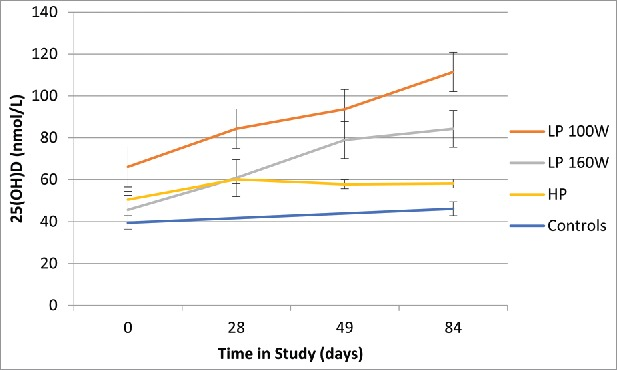
Source: PubMed
UVB phototherapy machine models
There are several models of NB-UVB phototherapy machines:
- The most common is the vertical booth used for office phototherapy, which has 24-48 lamps and is ideal for wide areas of lesions. However, the light intensity is less at the upper and lower ends of the lamps [12].
- Other models often used for home phototherapy include one-, two- and three-panel units, handsticks, hand, and foot units.
- Triple-panel units are most often prescribed for home phototherapy when a significant area of the body surface is involved, while hand wands are prescribed for the treatment of localized lesions [13].
What to consider in UV therapy
The treatment can last from four weeks to three months. To get the skin used to the radiation, the initial dose is determined according to the patient’s skin type, and then gradually increased.
During treatment, the patient’s eyes are protected with special sunglasses. Sensitive parts of the body not affected by psoriasis, such as the face or genitals, are covered to protect them. In addition, healthy skin can be protected by applying SPF 50+ sunscreen.
In keeping with current safety guidelines, the source is filtered to remove unnecessary UV radiation and is equipped with a timer to monitor the dose being administered. The 5-minute timer provides exposure to one standard erythemic dose (SED) at a distance of 20 inches from the user’s skin. The SED is a sub-erythemic dose for even the most sensitive type I human skin [14].
Possible side effects
Ultraviolet therapy can have various side effects. For example, radiation can dry out the skin and cause itching. Therefore, people are advised to thoroughly moisturize skin with skin care products that replenish lipids immediately after the treatment.
In people who get herpes on their lips, light therapy may increase the likelihood of herpes. Apply sunscreen to your lips before the treatment to prevent herpes.
Light therapy also often causes skin reactions similar to sunburns. In rare cases, blistering burns may occur. Other less common side effects include raised red spots that go away again after a few days, and hair follicle infections.
To limit side effects as much as possible, it is important to avoid natural sunlight on the day of treatment or to protect yourself outdoors by wearing appropriate clothing, sunglasses, and sunscreen.
Risks
Regular exposure to UV light increases your risk of skin cancer. The higher the dose of exposure and the more light therapy sessions you have, the higher the risk [1].
Narrow-band UVB phototherapy is probably associated with a lower risk of developing skin cancer. But this is not yet known for sure, because there are almost no studies on the risk of UVB-induced skin cancer.
The risk is also higher in people:
- with a lighter complexion;
- who have a history of skin cancer;
- who take medications to suppress their immune systems (immunosuppressants), such as azathioprine, cyclosporine, or methotrexate
To reduce the risk of skin cancer, the wavelength and dose of light used, as well as the duration of treatment, must be determined before starting treatment. Many different factors come into play here. It is important to see a skin specialist (dermatologist) who knows how to administer light therapy.

How to prepare for UV therapy
No deodorants and other things
On the day of treatment, do not use perfume, deodorants, aftershave lotions, or other cosmetic products.
Some of these contain substances that can make your skin more sensitive to light, and deodorant can even cause a spotty discoloration of the skin and take several months to disappear. Deodorant can be used after treatment.
About creams
On the days of the treatment, do not apply any creams or ointments to your skin before the treatment, except for a suitable water-based moisturizer. If you are not sure which creams or lotions are suitable, please consult a specialist.
Moisturize your skin one to two hours before the treatment, as this helps the skin absorb UV rays. Apply the moisturizer in smooth strokes in the direction of hair growth and allow the cream to absorb without rubbing it into the skin.
Do not use greasy creams, as they can cause burning and interfere with UV absorption. This will avoid conditions such as folliculitis, where the cream can get stuck in the root of the hair follicle and cause irritation and possibly infection.
Minimizing the risk of sunburn
During treatment, you should minimize the risk of sunburn: cover yourself with clothing with long sleeves, especially on sunny days, and wear a hat.
Use sunscreen with a factor of at least 20, which protects against UVA and UVB rays.

Home UVB Phototherapy Treatment
UV phototherapy is usually provided in an outpatient setting, so patients must come in for treatment two to three times a week during office hours. This is relatively time-consuming and often inconvenient for patients. To overcome these disadvantages, home UVB equipment exists. [15].
Home UVB phototherapy is as effective as outpatient UVB phototherapy for mild to severe psoriasis (DOT: Moderate) [4]. Such therapy usually requires brief exposure to UV radiation (usually a few minutes) every other day [16]. But it’s not that simple.
Although the literature shows that home phototherapy is well-tolerated, effective, and cost-effective, many dermatologists do not suggest home UVA as a treatment option for patients because of the perceived risks of treatment [12]. The risks of home phototherapy are low and comparable to outpatient treatment, but there is still the possibility of serious erythema, burns, or blisters [17].
Patients should receive detailed education on the use of home UV light, including treatment goals and how to recognize adverse reactions [18]. In addition, patient instructions should be individualized, given that each brand of phototherapy equipment has its own recommended treatment protocols, safety measures, and maintenance requirements.
The ideal situation is when patients starting home phototherapy have already had experience with outpatient phototherapy. Previous outpatient phototherapy experience provides an educational experience that reduces the risk of adverse events in the home department. Patients should follow instructions and understand the risks of treatment.
Summary
UVB therapy can be a real lifesaver for psoriasis, eczema, cutaneous lymphoma, vitiligo, polymorphic light rash, acne, and increasing vitamin D levels for patients with CF and SBS.
But UVB therapy can cause some side effects and increase the risk of skin cancer. That is why you should have your doctor determine the wavelength and dosage of the light used, as well as the duration of the treatment, before starting the treatment. It is also important to follow certain recommendations when using this therapy. Read more about them here.
Another disadvantage of UV therapy is that it requires a lot of doctor visits and is generally time-consuming. The solution to this problem is home UV therapy. However, if outpatient treatment is possible, it should be first-line therapy with closer monitoring and dose determination by a medical professional.
FAQ
💡 What is UVB treatment used for?
UVB therapy is used to treat psoriasis, eczema, cutaneous lymphoma, vitiligo, polymorphic light rash, acne, and increasing vitamin D levels for patients with CF and SBS.
🏠 Can I do phototherapy at home?
Yes, but although the literature shows that home phototherapy is well-tolerated, effective, and cost-effective, many dermatologists do not suggest home UVB radiation as a treatment option for patients because of the perceived risks of treatment.
🩺 Who is against UVB radiation therapy?
Regular exposure to UVB radiation increases the risk of skin cancer. The risk is higher in people with a fair complexion, people who have had skin cancer in the past, and those who take medications to suppress their immune systems (immunosuppressants) such as azathioprine, cyclosporine, or methotrexate. Before starting treatment, be sure to have a checkup with your doctor.
🥼 How can I reduce the risks from UVB phototherapy?
To reduce the risk of skin cancer, the wavelength and dose of light used, as well as the duration of treatment, must be determined before treatment begins. Many different factors come into play here. It is important to see a skin specialist (dermatologist) who knows how to administer light therapy.
🗓️ How long does UVB treatment last?
Treatment can last from four weeks to three months.
Sources
- Chen X, Yang M, Cheng Y, Liu GJ, Zhang M. Narrow-band ultraviolet B phototherapy versus broad-band ultraviolet B or psoralen-ultraviolet A photochemotherapy for psoriasis. Cochrane Database Syst Rev 2013; (10): CD009481
- Christoffers WA, Coenraads PJ, Svensson Å, Diepgen TL, Dickinson-Blok JL, Xia J, Williams HC. Interventions for hand eczema. Cochrane Database Syst Rev. 2019 Apr 26;4(4):CD004055. doi: 10.1002/14651858.CD004055.pub2. PMID: 31025714; PMCID: PMC6484375.
- Toledo-Pastrana T, García-Hernández MJ, Carrizosa-Esquivel AM, Camacho-Martínez FM. Evaluation of 25 years of phototherapy for treating psoriasis at a teaching hospital in southern Spain. An Bras Dermatol. 2015;90(4):473-8.
- Ontario Health (Quality). Home Narrowband Ultraviolet B Phototherapy for Photoresponsive Skin Conditions: A Health Technology Assessment. Ont Health Technol Assess Ser. 2020 Nov 2;20(12):1-134. PMID: 33240453; PMCID: PMC7668536.
- Chandra P, Wolfenden LL, Ziegler TR, Tian J, Luo M, Stecenko AA, Chen TC, Holick MF, Tangpricha V. Treatment of vitamin D deficiency with UV light in patients with malabsorption syndromes: a case series. Photodermatol Photoimmunol Photomed. 2007 Oct;23(5):179-85. doi: 10.1111/j.1600-0781.2007.00302.x. PMID: 17803596; PMCID: PMC2846322.
- Tangpricha V, Turner A, Spina C, Decastro S, Chen TC, Holick MF. Tanning is associated with optimal vitamin D status (serum 25-hydroxyvitamin D concentration) and higher bone mineral density. Am J Clin Nutr. 2004 Dec;80(6):1645-9. doi: 10.1093/ajcn/80.6.1645. PMID: 15585781.
- Webb AR, Kline L, Holick MF. Influence of season and latitude on the cutaneous synthesis of vitamin D3: exposure to winter sunlight in Boston and Edmonton will not promote vitamin D3 synthesis in human skin. J Clin Endocrinol Metab. 1988 Aug;67(2):373-8. doi: 10.1210/jcem-67-2-373. PMID: 2839537.
- Koutkia P, Lu Z, Chen TC, Holick MF. Treatment of vitamin D deficiency due to Crohn’s disease with tanning bed ultraviolet B radiation. Gastroenterology. 2001 Dec;121(6):1485-8. doi: 10.1053/gast.2001.29686. PMID: 11729127.
- Devgun MS, Johnson BE, Paterson CR. Tanning, protection against sunburn and vitamin D formation with a UV-A ‘sun-bed’. Br J Dermatol. 1982 Sep;107(3):275-84. doi: 10.1111/j.1365-2133.1982.tb00357.x. PMID: 6981420.
- Holick MF. Biological Effects of Sunlight, Ultraviolet Radiation, Visible Light, Infrared Radiation and Vitamin D for Health. Anticancer Res. 2016 Mar;36(3):1345-56. PMID: 26977036.
- Boston University School of Medicine. “LED lights safer, more effective in producing Vitamin D3 than sunlight.” ScienceDaily. ScienceDaily, 13 September 2017.
- Nolan BV, Yentzer BA, Feldman SR. A review of home phototherapy for psoriasis. Dermatol Online J. 2010;16:1
- Mohammad TF, Silpa-Archa N, Griffith JL, Lim HW, Hamzavi IH. Home phototherapy in vitiligo. Photodermatol Photoimmunol Photomed. 2017;33:241–252.
- Sayre RM, Dowdy JC, Shepherd JG. Reintroduction of a classic vitamin D ultraviolet source. J Steroid Biochem Mol Biol. 2007 Mar;103(3-5):686-8. doi: 10.1016/j.jsbmb.2006.12.062. Epub 2007 Feb 12. PMID: 17293107.
- Anstey A. Home UVB phototherapy for psoriasis. BMJ. 2009 May 7;338:b607. doi: 10.1136/bmj.b607. PMID: 19423624.
- Hum M, Kalia S, Gniadecki R. Prescribing Home Narrowband UVB Phototherapy: A Review of Current Approaches. J Cutan Med Surg. 2019 Jan/Feb;23(1):91-96. doi: 10.1177/1203475418800947. Epub 2018 Sep 15. PMID: 30221998.
- Koek MB, Buskens E, van Weelden H, Steegmans PH, Bruijnzeel-Koomen CA, Sigurdsson V. Home versus outpatient ultraviolet B phototherapy for mild to severe psoriasis: pragmatic multicentre randomised controlled non-inferiority trial (PLUTO study). BMJ. 2009 May 7;338:b1542. doi: 10.1136/bmj.b1542. PMID: 19423623; PMCID: PMC2679120.
- Gattu S, Pugashetti R, Koo J. The art and practice of UVB phototherapy and laser for the treatment of moderate-to-severe psoriasis. In: Koo J, Lee CS, Lebwohl MG, Weinstein GD, Gottlieb A, editors. Moderate to Severe Psoriasis. 3. New York, NY: Informa Healthcare; 2009. pp. 75–114.





Nice post. I used to be checking constantly this weblog and I am inspired!
Extremely helpful information particularly the last section 🙂 I take care of such information a lot.
I was seeking this certain info for a long time.
Thanks and good luck.